Hampshire's hospital services '˜under review' in bid to make them '˜sustainable'
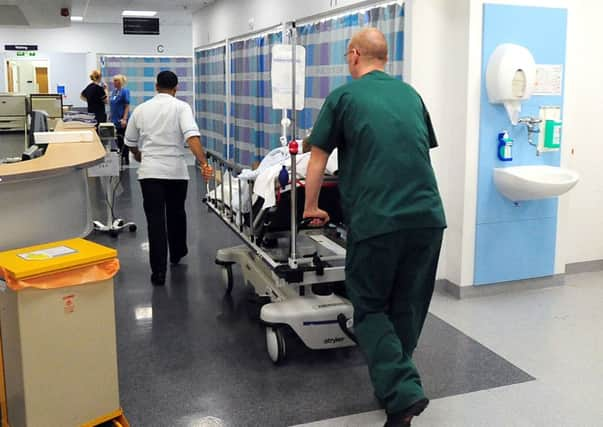

Under the changes, known as Sustainability and Transformation Plans, all services in acute hospitals – including Queen Alexandra Hospital – are under review.
NHS chiefs are proposing a Solent Acute Alliance – aiming to reduce the number of times patients will unnecessarily see medics, while also centralising services.
Advertisement
Hide AdAdvertisement
Hide AdThey hope to save £165m a year by 2020/21 across hospital services alone.
‘Care will be delivered locally where possible, but centrally where this improves outcomes,’ the plan says.
‘We will work with community providers allowing seamless services, and providing care and contact only when it offers best value.’
The services review includes: vascular, spinal, ear nose and throat, urology, haematology, colorectal surgery, maxillofacial surgery, paediatrics, neonatal intensive care unit, renal, gastroenterology, dermatology, oncology, cardiology, radiology and general surgery.
Advertisement
Hide AdAdvertisement
Hide AdNo decisions have been revealed yet and some services have not yet been reviewed under the plans.
Analysis of the STP documents show plans for:
n A cutback on the 8,000 surgical patients outsourced to the private sector by building more theatre at QA and Southampton in a bid to bring back 5,000 by 2020.
n Bringing in home-testing kits for some sexually-transmitted infections to cut down face-to-face appointments.
n A redesign of the paediatric intensive care unit service to have enough capacity.
Advertisement
Hide AdAdvertisement
Hide Adn Health care staff being given a ‘passport to work in Hampshire and the Isle of Wight’ meaning they can work outside their organisations across the county.
n Salvaging a ditched 2012 plan to consolidate pathology across acute hospitals to save £2m.
n The distribution and production facility for all pharmacy services at acute hospitals could be taken over by Portsmouth Hospitals NHS Trust.
n A patient portal for people to register their symptoms before being assessed, get ‘self-help’ and repeat prescriptions.
Advertisement
Hide AdAdvertisement
Hide AdAnd it comes as a confidential document, which lists most of the NHS buildings in the county, rates 39 in this area as being beyond economic life or surplus to requirement.
Inger Bird, estates lead for the Sustainability and Transformation Plan, said the list of buildings had been drawn up to give a picture of estates in the area – not necessarily meaning buildings will be sold off or shut. They could be refurbished.
‘If we were going to be making a decision where there is going to be a change in clinical services, that would be subject to consultation,’ she said.
‘None of that happens without that level of engagement.
‘The workbook is really just in order for us to be able to see what estates we’ve got, what do we need to work about and not work about and that’s really the aim of it.’
Advertisement
Hide AdAdvertisement
Hide AdDespite bidding to cut costs at every level, the document seen by The News – a confidential appendix to the STP – also reveals QA Hospital in Cosham, run under PFI, costs £383 per sq m to run each year – more than twice nearby Southampton General Hospital’s £171 per sq m cost.
QA costs £54.2m a year to run, compared to Southampton’s £39.4m a year.
However, the Southampton site is suffering a £34.3m maintenance backlog.
According to the plan, health chiefs also want to ‘sweat’ the county’s hospitals – making better use of space.
Advertisement
Hide AdAdvertisement
Hide AdIn Portsmouth, clinicians hope to set up three ‘cluster hubs’ serving sections of the city, called ‘local health hubs’.
‘These hubs will consolidate numerous existing premises into single sites helping to rationalise, and acquire best use of, public sector estate,’ one plan says.
Another adds: ‘These will provide extended access and an enhanced range of services which reduce the need for patients to travel to the main hospital.’
The hubs, serving areas of between 30,000 and 50,000 population, would be open from ‘8am and 8pm on weekdays, offering same-day access for urgent primary care, community and specialist clinics,an extended primary care team and wellbeing and illness prevention support,’ the STP said.
Advertisement
Hide AdAdvertisement
Hide AdLarger hubs called ‘area health hubs’ would serve either 200,000 or 100,000 population.
These would include, Gosport War Memorial Hospital, Petersfield Community Hospital, and Fareham Community hospital, which the are considered ready or only needing minor works.
Extra work is needed at St Mary’s Hospital in Portsmouth and Oak Park Community Clinic in Leigh Park to create the ‘area health hubs’, chiefs say.
But critics are not convinced the plans can be accomplished.
Advertisement
Hide AdAdvertisement
Hide AdCampaigner Jerry Brown said: ‘The STP was a good idea to start with but it got hijacked by the Department of Health and got turned into a money-saving exercise.
‘When that happened it got changed from being a plan from the front, to a plan from behind.
‘There’s the risk when five years on this hasn’t delivered, that we’re told by Department of Health that it was the NHS’s plan: “you wrote the plan, and haven’t delivered the plan so we’ve decided to get some people in”.’
Richard Samuel, who has drawn up Hampshire’s STP, defended the plans as intending keep the NHS going.
Advertisement
Hide AdAdvertisement
Hide AdHe said: ‘We can’t afford to do nothing, remembering we’re investing £0.3bn more into Hampshire and the Isle of Wight in the next four years.
‘It’s how do we spend that by doing something fundamentally different or spend it the same way and run into the same challenges.
‘Working with local medics and GPs, there are many, many who are gearing up to support people in different way at less cost with better outcomes.
‘As clinicians and clinical leaders we’ve all got to step up and find ways in which we can balance this.’
Advertisement
Hide AdAdvertisement
Hide AdThe buildings list, a confidential appendix to the STP, shows sections of St James Hospital, in Milton, are already on sale – but that their value have been hit by recent campaigns.
Solent NHS Trust is to spend around £11.3m on St Mary’s Health Campus when it brings the remaining St James’ services to the Milton Road campus.
Mark Young, head of estates at Solent NHS Trust, said: ‘We are now progressing plans to refurbish two blocks on the St Mary’s Community Health Campus
‘This work, scheduled to start in the new financial year, will provide new state of the art facilities and enable the relocation of some of our services currently located at St James Hospital.’
Advertisement
Hide AdAdvertisement
Hide AdHe added: ‘As well as providing a purpose-built environment for staff and patients, this significant project will incorporate new systems and ways of working that will enable better and more efficient use of NHS estate as set out in the region’s Sustainability Transformation Plan.
‘It will, in turn, also allow for the disposal of surplus NHS estate.’