Coronavirus: Portsmouth and Hampshire Covid-19 patients part of 'virtual wards' to help detect those getting sicker
and live on Freeview channel 276
The Covid Oximetry @home service has been launched across Portsmouth, West Hampshire and the Isle of Wight.
It sees patients with confirmed or suspected Covid given an oximeter to monitor and report their own blood oxygen levels to a healthcare team.
Advertisement
Hide AdAdvertisement
Hide AdLow blood oxygen levels, known as silent hypoxia, can be an early sign that patients are going to get sicker from the virus.
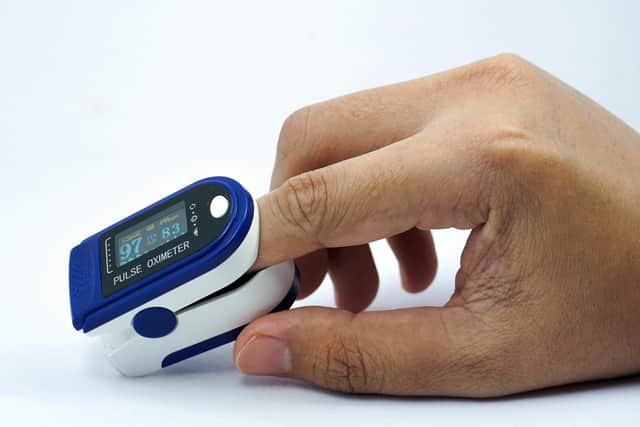

Normal levels are between 95 and 100 percent but anyone who has levels dropping below 92 per cent should go to A&E or call 999.
It is hoped the digital monitoring, also known as virtual wards, will help improve patient outcomes and reduce pressures on the NHS.
Clinical project lead, Dr Matt Inada-Kim, a consultant in acute medicine at Hampshire Hospitals, told the BBC Radio 4's Inside Health: ‘With Covid, we were admitting patients with oxygen levels in the 70s or low-or-middle 80s.
Advertisement
Hide AdAdvertisement
Hide Ad‘It was a really curious and scary presentation and really made us rethink what we were doing.
‘What we think we can see are the early seeds of a reduction in the length of stay after a hospital admission, an improvement in survival and a reduction in the pressures on the emergency services.’
There are 326 patients around Portsmouth, Fareham, Gosport and the South East Hampshire area who have been given an oximeter, which is a small device placed on the finger and beams of light pass through the blood in the finger to measure the amount of oxygen.
The programme, from Inhealthcare, is being rolled out across the rest of the county in primary, acute and out-of-hour settings.
Advertisement
Hide AdAdvertisement
Hide AdSarah Reese, director of transformation and delivery at the Hampshire and Isle of Wight Integrated Care System, spoke about the plan at Portsmouth City Council's Health Overview and Scrutiny Panel yesterday.
She said: ‘Virtual wards are very much as they say, virtual in nature. In general practice typically we identify patients that would benefit from some closer support and closer monitoring from primary care colleagues or through community colleagues.
‘They remain safely at home and we provide equipment where appropriate to monitor them and their oxygen levels for example so we can be really clear of the hour-by-hour state of those patients and our colleagues particularly in primary care and contact or visit any patients that needs it.’
A message from the Editor, Mark Waldron
You can subscribe here for unlimited access to Portsmouth news online - as well as fewer adverts, access to our digital edition and mobile app.
Our trial offer starts at just £2 a month for the first two months.
Comment Guidelines
National World encourages reader discussion on our stories. User feedback, insights and back-and-forth exchanges add a rich layer of context to reporting. Please review our Community Guidelines before commenting.