Health services in Portsmouth 'continuing to tackle' the Covid backlog as number of patients waiting for treatment breaks records again
and live on Freeview channel 276
New NHS England figures showed 46,383 patients were waiting for non-urgent elective operations or treatment at Portsmouth Hospitals University NHS Trust (PHU) at the end of March – up from 45,543 in February, and 36,653 in March 2021.
Of those, 864 (two per cent) had been waiting for longer than a year.
Advertisement
Hide AdAdvertisement
Hide AdAnd in the community 1,077 patients were waiting for non-urgent elective operations or treatment through Solent NHS Trust at the end of March – up from 1,042 in February, and 838 the same time last year.
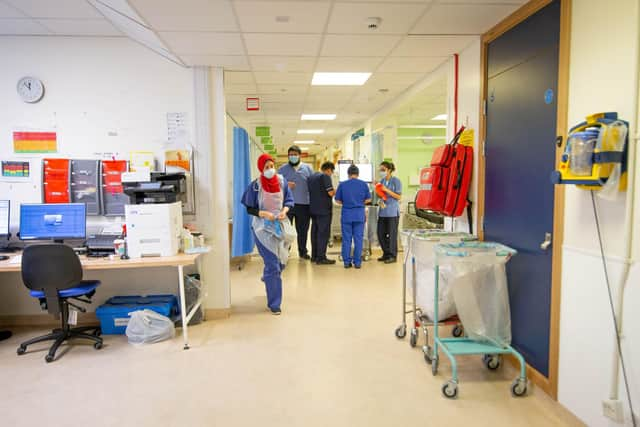

It mirrors the national trend as 6.4 million people were waiting to start treatment at the end of March – the highest number since records began in 2007.
Chief operating officer at PHU, Chris Evans, said: ‘We continue to tackle our Covid-19 backlog, while prioritising those who need urgent care.
‘Due to effective planning, maximising theatre utilisation and dedicated clinical engagement across our divisions, the trust has maintained its elective programme throughout the pandemic for those patients who were most unwell and those with the longest wait.


Advertisement
Hide AdAdvertisement
Hide Ad‘We currently have no patients waiting for elective treatment for more than 104 weeks and only two per cent have been waiting for more than a year.’
He added: ‘The trust has also expanded diagnostic testing capacity with the community diagnostic centre, based at St Mary’s Community Health Campus with additional hubs at Fareham Community Hospital and Oak Park Community Clinic in Havant.
‘This means more accessible and convenient services for our patients in a community setting and enables us to treat our most urgent patients in an acute setting when required.’
It comes as Queen Alexandra Hospital declared a critical incident on April 6 as all its beds were filled.
Advertisement
Hide AdAdvertisement
Hide AdAt the time there were reports that ambulances were having to wait outside for hours, unable to transfer patients.
This is reflected in the latest data from the South Central Ambulance Service (SCAS), which showed in April the average response time for life threatening situations was 9 minutes and 23 seconds – above the national standard of seven minutes and up from eight minutes 12 seconds the year before and six minutes and nine seconds in 2020.
Assistant director of operations for SCAS, Paul Jefferies, said: ‘All ambulance services across the UK are facing a challenging time with the impact of the Covid pandemic on staff sickness levels and rising patient demand not just for emergency 999 services but right across the NHS health system.
‘Despite these challenges, over the last 12 months, SCAS has been one of the top performing ambulance trusts for response times and consistently performed better than the average response times across England for all categories of emergency calls.
Advertisement
Hide AdAdvertisement
Hide Ad‘We continue working with our NHS partners to reduce the impact of hospital handover delays on our service and at times of peak demand and pressure, we as a Trust always focus on delivery of the safest and most responsive service to our most seriously ill and injured patients.’
He urged people to only call 999 in ‘life-threatening or serious cases’, saying ‘it will continue to be a challenging time for the NHS as we move into summer.’
‘For any urgent health problems, please use NHS 111 - either go online at 111.nhs.uk or call 111 - or the excellent range of urgent treatment centres, pharmacists and alternative NHS services in our region that are open from early in the morning till late at night every day, including weekends and bank holidays,’ he said.
Roger Batterbury, the chairman of health watchdog Healthwatch Portsmouth, said he understood that these are ‘incredibly difficult and worrying times’ for patients and carers.
Advertisement
Hide AdAdvertisement
Hide Ad‘We are aware that there are some regional plans to help mitigate this delay but we have no sense yet of when this might start and quite what this will look like if it is agreed,’ he said.
‘We get frequent calls to Healthwatch Portsmouth about the treatment delays and advise callers and anyone waiting that if their symptoms get worse to contact their GP surgeries as a first point of contact.
‘We are very aware of the local ambulance delays and have only in the last few days heard of a couple of cases of long delays which we have sent onto South Central Ambulance Service to investigate.
‘Our advice would be that if you are waiting for an emergency ambulance and the situation is getting worse to phone 999 to update them so they can reappraise their dispatch times.’
Advertisement
Hide AdAdvertisement
Hide AdSeparate figures showed 1.6 million patients in England were waiting for a key diagnostic test in March – a rise on 1.5 million in February.
At PHU, 12,328 patients were waiting for one of 12 standard tests, such as an MRI scan, non-obstetric ultrasound or gastroscopy at this time.
And at the Solent trust, 397 patients were waiting.
SEE ALSO: Doctor warns of rising monkeypox cases
Dan Baylis, chief medical officer at Solent NHS Trust, commented: ‘The restoration of services, including non-urgent treatment, scans and tests, and the reduction in the waiting times for our patients, is an absolute priority for us as we continue to ensure people receive high quality care when they need it.
‘While these figures show a slight increase in waiting times from February to March 2022, our teams continue to do everything possible to test, scan and treat people promptly.
Advertisement
Hide AdAdvertisement
Hide Ad‘Our proactive, strategic approach in managing the lists has seen us work with other local NHS organisations to increase the number of MRI and other scans available each month; we are also offering weekend appointments at the same time as ensuring high priority patients are seen at the earliest possible time.’
Comment Guidelines
National World encourages reader discussion on our stories. User feedback, insights and back-and-forth exchanges add a rich layer of context to reporting. Please review our Community Guidelines before commenting.
